Pain that starts as a mild ache during exercise but gradually worsens over time should never be ignored. For many active people, athletes, and even recreational exercisers, this kind of pain may signal a stress fracture—a common overuse injury that requires prompt diagnosis and proper management.
Stress fractures are more than just “minor bone pain.” Left untreated, they can worsen into serious injuries that delay recovery, limit mobility, and interfere with everyday life. The good news is that with early diagnosis, appropriate treatment, and expert rehabilitation, most stress fractures heal well and people can safely return to activity.
At Changez Health and Fitness, our multidisciplinary allied health team—including physiotherapists, exercise physiologists, dietitians, and personal trainers—works together to support every stage of recovery. Using our fully equipped rehabilitation gym, we help clients heal safely, restore strength, and return to the activities they love with confidence.
What Is a Stress Fracture?
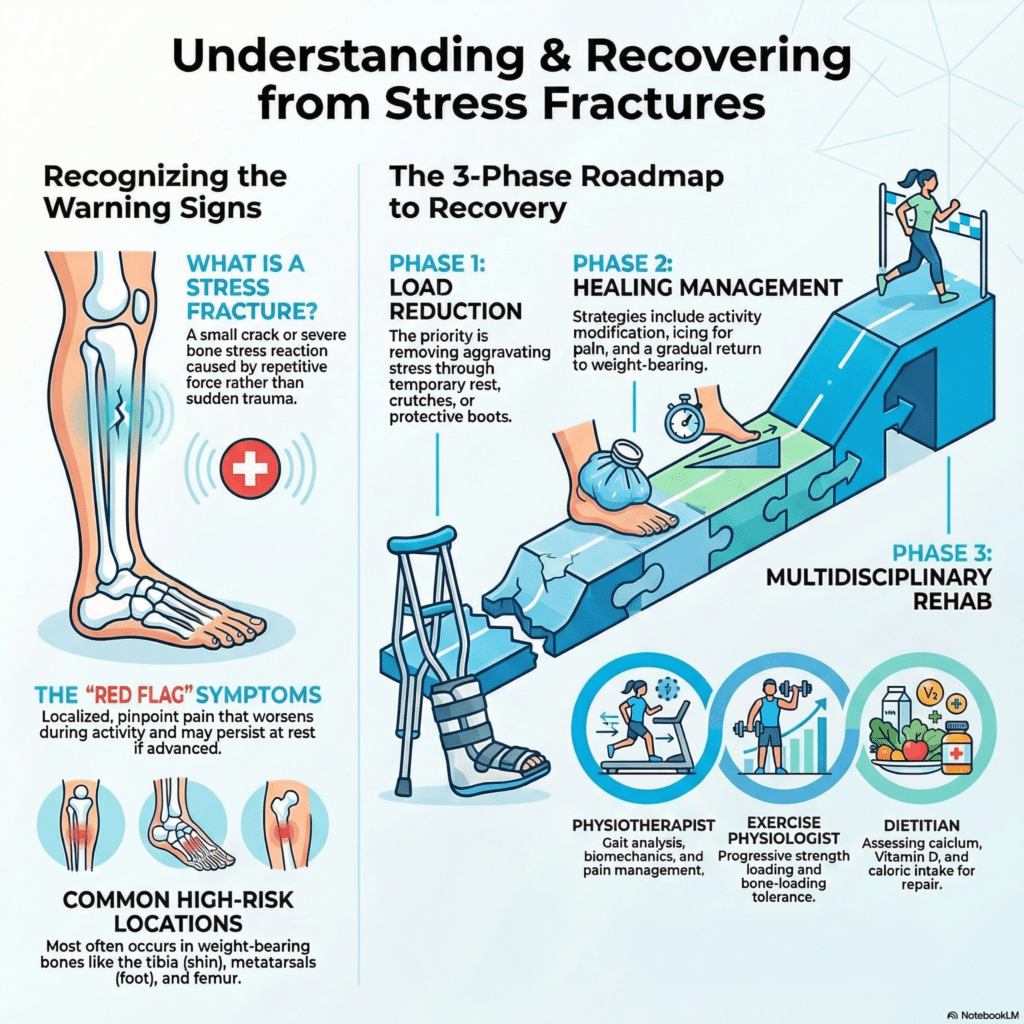
A stress fracture is a small crack or severe bone stress reaction caused by repetitive force or overuse rather than a sudden traumatic injury.
Unlike acute fractures caused by falls or accidents, stress fractures develop gradually over time when bones are repeatedly exposed to load without enough recovery to repair microscopic damage.
Bones are living tissue that constantly remodel under physical stress. Normally, this adaptation strengthens bone. However, when repetitive loading exceeds the body’s ability to recover, tiny cracks accumulate faster than bone can repair them.
This leads to a stress fracture.
Common Locations of Stress Fractures
Stress fractures most often occur in weight-bearing bones, including:
- Tibia (shin bone)
- Metatarsals (foot bones)
- Femur
- Pelvis
- Heel bone (calcaneus)
- Navicular bone in the foot
Athletes involved in running and jumping sports are especially vulnerable, but stress fractures can affect anyone who increases physical activity too quickly.
Who Is at Risk?
Stress fractures can happen to both athletes and non-athletes. Common risk groups include:
Athletes and Runners
Repetitive impact loading increases bone strain.
People Returning to Exercise Too Quickly
Rapid increases in training volume can overload bones.
Military Recruits
Sudden increases in marching and load-bearing activity create high risk.
Women with Hormonal Imbalances
Low energy availability and menstrual irregularities can weaken bone health.
Older Adults with Reduced Bone Density
Osteopenia and osteoporosis raise fracture susceptibility.
Individuals with Nutritional Deficiencies
Low calcium, vitamin D, or inadequate calorie intake can impair bone repair.
Causes of Stress Fractures
Several factors contribute to stress fracture development:
- Training Errors
Increasing intensity, duration, or frequency too rapidly.
- Poor Footwear
Unsupportive shoes reduce shock absorption.
- Biomechanical Issues
Flat feet, poor gait mechanics, or muscle imbalances increase abnormal load.
- Weak Muscles
Fatigued muscles transfer greater stress onto bones.
- Low Bone Density
Weaker bones tolerate less repetitive stress.
- Inadequate Recovery
Insufficient rest between training sessions limits healing time.
Symptoms of a Stress Fracture
Stress fractures often begin subtly.
Typical symptoms include:
- Localised pain during activity
- Pain that worsens with continued exercise
- Tenderness over a specific bone
- Swelling in the affected area
- Pain that may persist even at rest if advanced
Unlike muscle soreness, stress fracture pain is usually highly specific and reproducible when pressure is applied.
Ignoring these warning signs can worsen the injury.
How Are Stress Fractures Diagnosed?
Early diagnosis is essential to prevent progression.
Clinical Assessment
A physiotherapist or medical practitioner will assess:
- Pain history
- Activity changes
- Training load patterns
- Tenderness location
- Functional movement limitations
Imaging Tests
X-rays
Often first-line, but may miss early-stage fractures.
MRI
Gold standard for early detection; highly sensitive.
Bone Scan
Sometimes used if MRI is unavailable.
CT Scan
Helpful for complex or high-risk fracture sites.
Because some stress fractures are not visible on early X-rays, clinical suspicion remains extremely important.
Why Early Diagnosis Matters
If untreated, stress fractures may progress into:
- Complete fractures
- Prolonged healing times
- Chronic pain
- Surgical intervention in severe cases
High-risk fracture sites, such as the navicular bone or femoral neck, require urgent management to avoid complications.
Treatment of Stress Fractures
Treatment depends on location, severity, and individual risk factors.
Phase 1: Load Reduction
The first priority is removing aggravating stress.
This may involve:
- Stopping impact activity temporarily
- Using crutches if needed
- Wearing protective boots or braces
Rest does not always mean total inactivity—cross-training may still be appropriate.
Phase 2: Pain and Healing Management
Healing strategies may include:
- Activity modification
- Ice for pain relief
- Gradual weight-bearing progression
- Monitoring symptoms carefully
Most low-risk stress fractures heal within 6–8 weeks, though some require longer.
Phase 3: Rehabilitation and Reconditioning
This is where allied health becomes critical.
Rest alone is not enough.
Without correcting underlying causes, recurrence risk remains high.
How Changez Allied Health Professionals Help
At Changez Health and Fitness, recovery is team-based and comprehensive.
Physiotherapists: Diagnosis, Pain Management, and Biomechanics
Our physiotherapists:
- Identify movement dysfunctions
- Assess gait and loading mechanics
- Guide pain management strategies
- Assist safe return-to-movement planning
They help determine why the injury occurred—not just where it hurts.
Exercise Physiologists: Strength and Progressive Reloading
Exercise physiologists design structured rehabilitation programs that:
- Restore muscular strength
- Improve bone-loading tolerance
- Rebuild balance and coordination
- Gradually reintroduce functional exercise safely
This progression is essential for long-term bone resilience.
Dietitians: Bone Healing Through Nutrition
Nutrition is often overlooked in fracture healing.
Our dietitians assess:
- Calcium intake
- Vitamin D adequacy
- Protein requirements
- Energy availability
Poor nutrition delays bone repair and increases reinjury risk.
Personal Trainers: Safe Return to Exercise in Our Fully Equipped Gym
Once medically cleared, personal trainers help clients:
- Rebuild confidence
- Regain fitness safely
- Return to sport progressively
- Maintain conditioning during transition phases
Our fully equipped gym allows tailored rehabilitation in a supervised environment.
The Importance of Multidisciplinary Care
Stress fractures are rarely caused by one factor alone.
Successful recovery often requires addressing:
- Bone health
- Muscle weakness
- Biomechanical inefficiencies
- Training errors
- Nutritional deficits
This is why integrated allied health care achieves better outcomes than isolated treatment alone.
Returning to Exercise After a Stress Fracture
Returning too soon can restart injury cycles.
A gradual progression is critical.
Typical return includes:
- Pain-free walking
- Strength restoration
- Low-impact cross-training
- Gradual loading drills
- Controlled return-to-run programs
Each stage must be symptom-monitored carefully.
Preventing Future Stress Fractures
Prevention strategies include:
- Increasing training loads gradually
- Wearing proper footwear
- Addressing biomechanical issues early
- Maintaining adequate nutrition
- Strength training regularly
- Allowing proper recovery time
Bone adapts best to progressive, consistent loading—not sudden spikes.
Why Strength Training Matters in Prevention
Strength training improves:
- Bone density
- Muscular shock absorption
- Joint stability
- Movement efficiency
Strong muscles reduce repetitive bone overload and protect against reinjury.
At Changez, strength programs are customised for each client’s sport, age, and injury history.
When to Seek Professional Help
You should seek assessment if:
- Pain persists beyond a few days
- Pain worsens with activity
- Swelling develops
- Pain becomes pinpoint and localised
Early intervention leads to faster recovery and fewer complications.
How Changez Health and Fitness Supports Your Recovery
At Changez Health and Fitness, we specialise in evidence-based rehabilitation that combines clinical expertise with practical gym-based recovery.
Our stress fracture rehabilitation services include:
- Comprehensive injury assessment
- Physiotherapy diagnosis and treatment
- Exercise physiology rehabilitation plans
- Nutritional bone health support
- Supervised strength rebuilding
- Safe return-to-sport programs
Whether you are an athlete, weekend runner, dancer, walker, or active older adult, our team helps you recover smarter—not just faster.
Final Thoughts
Stress fractures are common but highly manageable when identified early and treated correctly.
Ignoring persistent bone pain can turn a small injury into a major setback. With timely diagnosis, structured rehabilitation, and multidisciplinary support, most people recover fully and return stronger than before.
At Changez Health and Fitness, our expert allied health team works together to treat the whole person—not just the injury—helping clients heal safely, prevent recurrence, and return confidently to movement.
Because recovery is not just about healing bones—it is about rebuilding strength for life.
References
Brukner, P., & Khan, K. (2019). Brukner & Khan’s Clinical Sports Medicine (5th ed.). McGraw-Hill.
Bennell, K. L., Malcolm, S. A., Thomas, S. A., et al. (1996). Risk factors for stress fractures in track and field athletes. The American Journal of Sports Medicine, 24(6), 810–818.
American Academy of Orthopaedic Surgeons. (2024). Stress fractures. https://orthoinfo.aaos.org
Healthy Bones Australia. (2024). Bone stress injuries and prevention. https://healthybonesaustralia.org.au