A Capacity-Based Approach at Changez Health & Fitness Daisy Hill
Tendon pain is one of the most common — and most misunderstood — musculoskeletal conditions affecting runners, field sport athletes, gym-goers, and active adults.
Achilles. Patellar. Gluteal. Proximal hamstring. Rotator cuff.
Many people are told the same thing:
“Just rest.”
And while short-term load reduction may settle symptoms, rest alone rarely resolves tendinopathy long term.
In fact, prolonged rest can reduce tendon capacity, delay return to activity, and increase the risk of recurrence when sport or exercise resumes.
At Changez Health & Fitness in Daisy Hill, we take a different approach — one grounded in modern tendon science:
Tendons need progressive load to recover.
Understanding Tendinopathy: It’s Not Just “Inflammation”
Historically, tendon pain was labelled “tendinitis,” implying inflammation as the primary driver.
However, research over the past two decades shows that most chronic tendon pain is not primarily inflammatory. Instead, it reflects a load-related tendon adaptation issue.
Cook & Purdam’s continuum model of tendinopathy describes tendon pathology as a response to excessive or poorly managed load. Tendons adapt positively when load is appropriate. They become reactive and painful when load exceeds capacity.
This means:
- Too much load too quickly → pain
- Too little load for too long → reduced capacity
- Appropriate progressive load → adaptation and resilience
Rest may calm symptoms temporarily, but it does not rebuild the tendon’s ability to tolerate stress.
And if capacity isn’t restored, symptoms often return when activity resumes.
Why Rest Alone Often Fails
Tendons Adapt to Mechanical Load
Tendon tissue is living, dynamic, and responsive to stress.
Mechanical loading stimulates:
- Collagen synthesis
- Improved tendon stiffness
- Increased force transmission capacity
- Neuromuscular improvements
Complete rest removes that stimulus.
Without load:
- Tendon stiffness decreases
- Muscle strength declines
- Reactive capacity reduces
- Confidence drops
The result? When activity resumes, the tendon is less prepared than before.
Pain Reduction ≠ Capacity Restoration
One of the biggest mistakes in tendon rehab is equating pain relief with recovery.
Pain may settle with:
- Rest
- Anti-inflammatory medication
- Corticosteroid injection
- Reduced training load
But unless strength and load tolerance are rebuilt, the underlying issue remains.
This explains the common cycle:
Rest → Feel better → Return to sport → Flare-up → Rest again.
Breaking this cycle requires progressive capacity development.
The Evidence: Progressive Loading Works
Across Achilles, patellar, gluteal and hamstring tendinopathies, the strongest evidence supports structured, progressive loading programs.
Patellar Tendinopathy
Progressive tendon-loading programs have demonstrated superior long-term improvements in VISA scores compared to traditional eccentric-only approaches.
Modern staged programs typically include:
- Isometrics (for pain modulation)
- Isotonic loading (strength development)
- Energy storage and release (plyometrics)
- Sport-specific reconditioning
This staged progression better reflects real sporting demands.
Achilles Tendinopathy
Clinical guidelines consistently support exercise therapy as first-line management.
Successful programs emphasise:
- Heavy slow resistance
- Progressive calf loading
- Monitoring symptom response
- Gradual reintroduction of running
Research shows recurrence risk is highest during the return-to-sport phase — precisely when many athletes progress too quickly without structured guidance.
Gluteal Tendinopathy
The LEAP trial (conducted in Australia) demonstrated that education combined with exercise outperformed corticosteroid injection at both short- and long-term follow-up.
Key principles included:
- Load management education
- Progressive hip strengthening
- Avoidance of compressive aggravators early
- Gradual exposure to higher-demand activity
Again, rest alone was not the solution.
Proximal Hamstring Tendinopathy
Although the evidence base is smaller, expert consensus supports:
- Education
- Progressive posterior chain strengthening
- Graded speed and sprint reintroduction
Long-term success depends on restoring hamstring load tolerance — not eliminating load altogether.
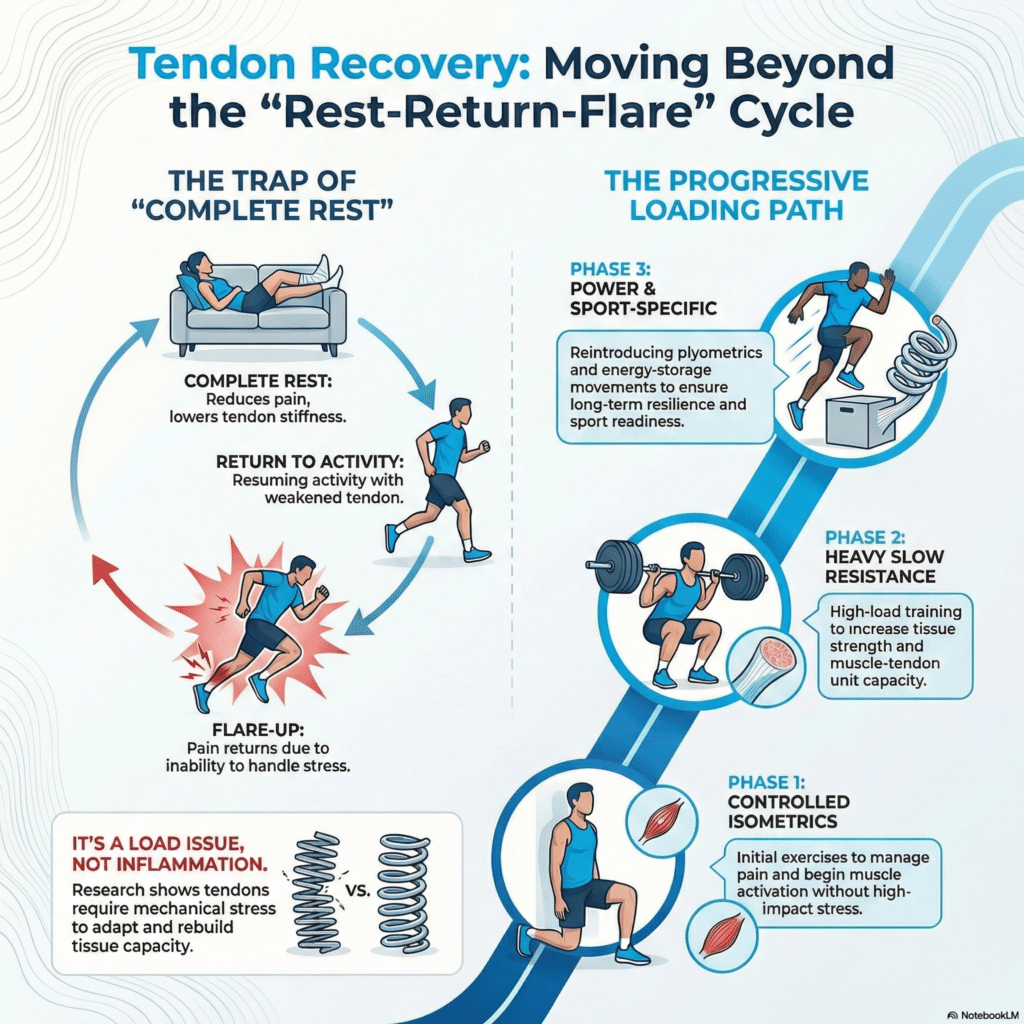
Why Tendon Rehab Must Be Progressive
Tendon rehabilitation follows a logical sequence:
Stage 1: Calm the Reactive Phase (Not Total Rest)
- Relative load modification
- Isometric loading (analgesic effect)
- Avoid complete unloading
The goal is symptom control without deconditioning.
Stage 2: Rebuild Strength
- Heavy slow resistance
- Controlled tempo work
- Progressive overload
This stage restores:
- Muscle force capacity
- Tendon stiffness
- Load tolerance
Stage 3: Energy Storage & Release
This is where many home programs fall short.
Sport and running demand:
- Plyometrics
- Deceleration control
- Stretch-shortening cycle efficiency
- Repeated loading tolerance
These demands must be trained progressively.
Stage 4: Return to Sport / Running
Criteria-based progression may include:
- Strength symmetry benchmarks
- Reactive strength testing
- Cumulative load tolerance
- Fatigue resilience
Without these objective checkpoints, progression becomes guesswork.
Why Supervised Gym-Based Rehab Is More Effective
Direct head-to-head trials comparing supervised versus home-based rehab across all tendon types are limited.
However, we know the critical ingredients for success:
✔ Progressive heavy loading
✔ Objective progression criteria
✔ Load monitoring
✔ Movement correction
✔ Sport-specific reconditioning
These are far easier to deliver in a supervised, fully equipped environment.
At Changez Health & Fitness Daisy Hill, we can:
- Load heavy enough to stimulate adaptation
- Adjust load in real time
- Monitor technique
- Integrate conditioning
- Progress plyometrics safely
- Track measurable improvements
Many home programs fail simply because they cannot deliver sufficient loading stimulus.
Why Injections Alone Don’t Solve the Problem
Corticosteroid injections may reduce pain short term.
However:
- They do not rebuild tendon capacity.
- Recurrence rates are often high.
- Structural adaptation does not occur.
Long-term success depends on restoring mechanical tolerance.
Load builds resilience.
Tendinopathy in Runners: The Flare-Up Trap
Runners frequently fall into the boom-bust cycle:
- Rest completely
- Resume full mileage
- Flare
- Rest again
This pattern delays adaptation.
Instead, we use graded return-to-run models based on:
- Symptom monitoring rules
- Calf endurance benchmarks
- Reactive strength tolerance
- Progressive mileage increments
Consistency, not perfection, drives recovery.
The Changez Tendon Rehab Model
At Changez Health & Fitness in Daisy Hill, our approach integrates physiotherapy, exercise physiology, and structured gym-based progression.
Comprehensive Assessment
We assess:
- Tendon load history
- Strength deficits
- Kinetic chain contributors
- Movement mechanics
- Training errors
Diagnosis guides progression.
Individualised Progressive Loading
Depending on tendon type, programs may include:
- Heavy calf raises
- Leg press variations
- Hip thrusts
- Hamstring strengthening
- Tempo-controlled resistance
- Sled pushes
- Landmine loading
- Isometric pain modulation drills
Progression is data-driven, not symptom-driven alone.
Objective Monitoring
We track:
- Strength capacity
- Repetition tolerance
- Reactive strength
- Symptom response to cumulative load
- Running progression markers (if relevant)
You do not “hope” you’re improving.
You measure it.
Multidisciplinary Support
Physiotherapy:
- Diagnosis
- Load modification strategy
- Pain education
- Return-to-sport rules
Exercise Physiology:
- Progressive overload
- Conditioning maintenance
- Strength deficits correction
- Energy storage integration
Dietetics (when required):
- Protein optimisation
- Energy availability
- Recovery nutrition
Tendon adaptation requires both mechanical and metabolic support.
Common Myths About Tendinopathy
Myth 1: Stretching fixes tendon pain
Stretching alone rarely resolves load-related tendon pathology.
Myth 2: Pain means damage is worsening
Pain during controlled loading does not necessarily indicate structural harm.
Myth 3: You must avoid pain entirely
Mild, monitored discomfort during rehab can be acceptable and part of adaptation.
Myth 4: Rest is safest
Prolonged rest can reduce capacity and increase recurrence risk.
When Should You Seek Assessment?
- Pain lasting more than 2–3 weeks
- Recurrent flare-ups
- Morning stiffness that persists
- Pain during sport that worsens over time
- Difficulty progressing mileage or training load
Early intervention prevents chronic progression.
Tendinopathy Treatment in Daisy Hill
If you are searching for:
- Achilles tendinopathy physiotherapy Daisy Hill
- Patellar tendon rehab Logan
- Gluteal tendinopathy treatment Brisbane Southside
- Return to running after tendon pain
- Progressive loading rehab
Changez Health & Fitness provides structured, evidence-aligned rehabilitation under one roof.
The Bottom Line: Load Is Medicine
Tendons do not get stronger from avoidance.
They get stronger from progressive, intelligent loading.
Rest alone may reduce symptoms temporarily — but it does not restore resilience.
If you are caught in the cycle of flare-ups, inconsistent training, and frustration, it is likely not a motivation problem.
It is a capacity problem.
And capacity can be built.
Build Capacity. Move Confidently. Stay Active.
At Changez Health & Fitness in Daisy Hill, we help active adults and athletes:
- Break the flare-up cycle
- Rebuild tendon resilience
- Return to consistent training
- Reduce recurrence risk
Book a Tendon Assessment today.
Stronger tissue.
Smarter loading.
Long-term outcomes.
References
Cook, J. L., & Purdam, C. R. (2009). Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. British Journal of Sports Medicine, 43(6), 409–416. https://doi.org/10.1136/bjsm.2008.051193
Docking, S. I., & Cook, J. (2015). Pathological tendons maintain sufficient aligned fibrillar structure on ultrasound tissue characterisation (UTC). Scandinavian Journal of Medicine & Science in Sports, 25(3), e222–e230. https://doi.org/10.1111/sms.12291
Goom, T. S., Malliaras, P., Reiman, M. P., & Purdam, C. (2016). Proximal hamstring tendinopathy: Clinical aspects of assessment and management. Journal of Orthopaedic & Sports Physical Therapy, 46(6), 483–493. https://doi.org/10.2519/jospt.2016.5986
Kongsgaard, M., Kovanen, V., Aagaard, P., Doessing, S., Hansen, P., Laursen, A. H., … Magnusson, S. P. (2009). Corticosteroid injections, eccentric decline squat training and heavy slow resistance training in patellar tendinopathy. The American Journal of Sports Medicine, 37(4), 790–802. https://doi.org/10.1177/0363546508330125
Malliaras, P., Barton, C. J., Reeves, N. D., & Langberg, H. (2013). Achilles and patellar tendinopathy loading programmes: A systematic review comparing clinical outcomes and identifying potential mechanisms for effectiveness. Sports Medicine, 43(4), 267–286. https://doi.org/10.1007/s40279-013-0019-z
Mellor, R., Grimaldi, A., Wajswelner, H., Hodges, P., Littlewood, C., Hall, M., … Vicenzino, B. (2018). Exercise and load modification versus corticosteroid injection versus wait and see for persistent gluteal tendinopathy (LEAP trial): A randomised clinical trial. BMJ, 361, k1662. https://doi.org/10.1136/bmj.k1662
Rio, E., Kidgell, D., Purdam, C., Gaida, J., Moseley, G. L., Pearce, A. J., & Cook, J. (2015). Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. British Journal of Sports Medicine, 49(19), 1277–1283. https://doi.org/10.1136/bjsports-2014-094386
Silbernagel, K. G., Hanlon, S., & Sprague, A. (2020). Current clinical concepts: Conservative management of Achilles tendinopathy. Journal of Athletic Training, 55(5), 438–447. https://doi.org/10.4085/1062-6050-356-19
van Ark, M., Zwerver, J., van den Akker-Scheek, I., & others. (2021). Progressive tendon-loading exercise therapy for patellar tendinopathy: A randomised clinical trial. British Journal of Sports Medicine, 55(9), 501–509. https://doi.org/10.1136/bjsports-2020-103403
Warden, S. J., Davis, I. S., & Fredericson, M. (2014). Management and prevention of bone stress injuries in long-distance runners. Journal of Orthopaedic & Sports Physical Therapy, 44(10), 749–765. https://doi.org/10.2519/jospt.2014.5334


